Gout is one of the oldest known forms of arthritis and develops when uric acid builds up in the body, forming sharp crystals in the joints. It often affects the big toe and can appear suddenly with intense pain, redness, warmth, and swelling. Attacks may come on overnight and make even light pressure feel unbearable. Several risk factors can increase the chance of gout, including a family history of the condition, frequent alcohol consumption, and diets high in red meat or sugary drinks. Obesity and certain medical conditions can also play a role. A podiatrist can identify gout, manage painful flare-ups, and work with patients to reduce joint damage and improve mobility. If you have intense pain in your big toe, it is suggested that you consult a podiatrist who can offer you a diagnosis and appropriate treatment.
Gout is a foot condition that requires certain treatment and care. If you are seeking treatment, contact Tanya R. Sellers-Hannibal, DPM from Maryland. Our doctor will treat your foot and ankle needs.
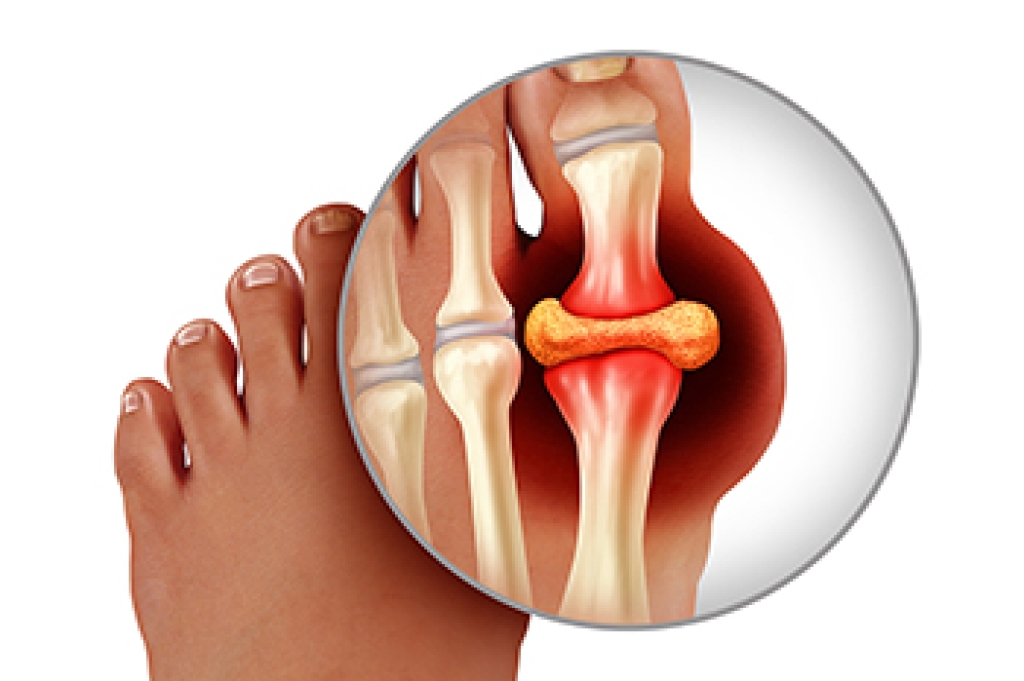
What Is Gout?
Gout is a type of arthritis caused by a buildup of uric acid in the bloodstream. It often develops in the foot, especially the big toe area, although it can manifest in other parts of the body as well. Gout can make walking and standing very painful and is especially common in diabetics and the obese.
People typically get gout because of a poor diet. Genetic predisposition is also a factor. The children of parents who have had gout frequently have a chance of developing it themselves.
Gout can easily be identified by redness and inflammation of the big toe and the surrounding areas of the foot. Other symptoms include extreme fatigue, joint pain, and running high fevers. Sometimes corticosteroid drugs can be prescribed to treat gout, but the best way to combat this disease is to get more exercise and eat a better diet.
If you have any questions, please feel free to contact our office located in Owings Mills, MD . We offer the newest diagnostic and treatment technologies for all your foot care needs.