Connect With Us

Blisters on the Feet
Blisters are a common ailment of people who wear shoes that are either too tight or rub against the feet in an uncomfortable way. Knowing the basics of blisters is important for understanding how they are formed and what treatments should be used for them.
A blister on the foot, or any other part of the body, is a small pocket that is filled with fluid. It usually forms on the upper layer of the skin because these layers are loose enough to allow a blister to form. The most common fluid in a blister is just a clear, watery-like fluid that usually isn’t cause for concern. However, blisters can fill up with blood if they are deep enough and pus if they have become infected with bacteria.
Blisters almost always form on the feet due to shoes rubbing up against the foot, where the friction causes blisters. These can occur after you have walked for a long period of time or when your shoes do not fit you properly. Your feet are also more prone to blisters if they are moist, so keeping them dry and clean is one preventative step you can take.
Preventing infection should be the number one concern when treating blisters, as well as relieving the pain they can cause. Using a bandage to cover up the blister will help it heal and prevent bacteria from entering it. New skin will form under the blister and eventually cause it to pop. You can also take a sterilized pin and try to pop it yourself.
If the blister is filled with pus or blood, seeking treatment from a doctor is ideal. Antibiotics may need to be taken in order to completely eliminate the bacteria inside the blister. See a doctor to have an antibiotic prescribed.
The best way to treat blisters is to prevent them all together. Keeping your feet dry and making sure that your shoes fit properly are just two of the steps you can take to prevent blisters. Shoes that are too tight or shoes that are too loose and allow your feet to slide in them will cause blisters. Applying a bandage to an area where you think a blister is about to form is another way you can prevent them.
Pregnancy and Foot Health
Many pregnant women complain about foot pain while they are expecting. Foot pain can primarily be caused by weight gain and hormonal changes taking place in the body. By understanding how pregnancy impacts the health of a woman's feet, a pregnant woman can take action to keep her feet as healthy and comfortable as possible.
Because a woman's weight changes during pregnancy, more pressure is brought to bear on both the legs and the feet. This weight shift can cause two major foot problems: over-pronation, also known as flat feet, as well as edema, which is swelling of the feet. Over-pronation occurs when the arch of the foot flattens, causing the foot to roll inwards when the individual is walking, and can aggravate the plantar fascia tissues located along the bottom of the feet. If these tissues become inflamed, a pregnant woman can experience pain in the heel of the foot as well as severe foot pain while walking or standing. Swelling of the feet, or edema, often occurs in the later stages of pregnancy. It is caused by slow circulation and water retention, and may turn the feet a light purple color.
To keep feet in good health and prevent over-pronation, pregnant women should avoid walking barefoot and be sure they are wearing shoes that offer good arch support. A device known as an orthotic can be added to regular footwear in order to provide additional support for the feet during pregnancy. Any expectant mother whose feet hurt should first check to see if the shoes she is wearing are old, worn out and not offering the proper support necessary for distributing the weight of her body during pregnancy.
To treat edema of the feet, a good start is to wear quality footwear which offers support and good circulation. Keep feet elevated whenever possible by using a foot stool while seated. Stay well hydrated by drinking plenty of water to prevent water retention in the feet. Any swelling that occurs in only one foot should be examined as soon as possible by a doctor.
Good foot health during pregnancy can help expectant mothers avoid foot pain that leads to other health problems. Massaging the feet and doing regular gentle exercise like walking aids foot health by contributing to good circulation. Supportive shoes are also a good investment that will support foot health during pregnancy.
Foot Conditions Can Develop From Playing Pickleball

Pickleball is a trending sport that many people enjoy. As with any physical sport, there can be painful foot repercussions if care is not taken while playing pickleball. Two common conditions that can be associated with this activity are plantar fasciitis and Achilles tendinitis. The ligament that runs along the bottom of the foot from the heel to the toes is called the plantar fascia. The fibers from the Achilles tendon run into the plantar fascia. The Achilles tendon attaches to the back of the heel and the plantar fascia on the bottom. The condition known as plantar fasciitis is when the plantar fascia becomes overstretched or sustains micro tears and causes pain in the heel area, especially when first steps are taken after prolonged rest. Achilles tendinitis is often an overuse injury as well. These things can happen after playing pickleball. Stretching the feet and calves, wearing supportive and well-fitting footwear, and resting the affected areas can all help. If the pain you feel in the heel or Achilles tendon continues or worsens, it is suggested that you seek the counsel of a podiatrist. This foot care expert can diagnose and treat foot pain and provide additional suggestions on how you might prevent foot problems while playing pickleball.
Sports related foot and ankle injuries require proper treatment before players can go back to their regular routines. For more information, contact Tanya R. Sellers-Hannibal, DPM of Maryland. Our doctor can provide the care you need to keep you pain-free and on your feet.
Sports Related Foot and Ankle Injuries
Foot and ankle injuries are a common occurrence when it comes to athletes of any sport. While many athletes dismiss the initial aches and pains, the truth is that ignoring potential foot and ankle injuries can lead to serious problems. As athletes continue to place pressure and strain the area further, a mild injury can turn into something as serious as a rupture and may lead to a permanent disability. There are many factors that contribute to sports related foot and ankle injuries, which include failure to warm up properly, not providing support or wearing bad footwear. Common injuries and conditions athletes face, including:
- Plantar Fasciitis
- Plantar Fasciosis
- Achilles Tendinitis
- Achilles Tendon Rupture
- Ankle Sprains
Sports related injuries are commonly treated using the RICE method. This includes rest, applying ice to the injured area, compression and elevating the ankle. More serious sprains and injuries may require surgery, which could include arthroscopic and reconstructive surgery. Rehabilitation and therapy may also be required in order to get any recovering athlete to become fully functional again. Any unusual aches and pains an athlete sustains must be evaluated by a licensed, reputable medical professional.
If you have any questions please feel free to contact our office located in Owings Mills, MD . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Sports Related Foot And Ankle Injuries
Foot and ankle injuries are common among people who participate in sports. Several factors contribute to this. They include failing to stretch or warm up properly, not wearing the proper type of shoe and not taping or providing other types of support for the ankle or foot. The most common foot and ankle injuries suffered by people involved in sports are plantar fasciitis, ankle sprains and Achilles tendon damage or ruptures. If not treated properly, they can lead to permanent disability.
Treating these injuries is relatively simple if they are identified and addressed early. Many athletes dismiss the initial aches and pains associated with injury as just soreness or tired muscles. Their first response is usually to try to work through it. This can lead to serious problems. Many minor injuries are made far more serious when athletes continue to put strain and pressure on them. That attitude can change a mild strain into a serious strain and a minor tear into a rupture. Athletes should have unusual aches and pains evaluated by a skilled medical professional.
Plantar fasciitis is a painful injury. It is inflammation of the plantar fascia, the thick band of tissue running from the heel to the base of the toes. If left untreated, it can lead to a degenerative disease called plantar fasciosis. There are several effective treatments for this ailment. Doctors often prescribe rest, massages, stretching, night splints, physical therapy, anti-inflammatory medication, corticosteroids or surgery, usually in that order. The most effective treatment for plantar fasciitis is orthotics, which offers foot support. Surgery is occasionally used as a last resort, but it comes with the risk of nerve damage and infection and often does not stop the pain.
The Achilles tendon is the largest tendon in the body. It connects the calf muscles to the heel bone. Running, jumping and walking all impact this tendon. Two common injuries to the Achilles tendon are tendonitis and a rupture of the tendon. Tendonitis is inflammation in the tendon often caused by an increase in the amount of stress placed on it. Non-surgical treatments include rest, ice or anti-inflammatory medication. A rupture (tear) of the Achilles tendon can be treated by placing the lower leg in a cast for several weeks or with surgery. Many physicians feel surgery is the better option because it lowers the risk of re-ruptures. Both methods require 4 to 6 months of rehabilitation.
Ankle sprains are the most common sports related foot and ankle injury. A sprain occurs when the ligament holding the ankle bones and joint stretches beyond its normal range. It can be treated non-surgically with a combination of rest, ice wrapped around the joint for 30 minutes immediately after injury, compression by a bandage and elevating the ankle above the heart for 48 hours. This combination is referred to as RICE. Severe ankle sprains in which the ligaments are torn may require reconstructive surgery followed by rehabilitation.
What Is a Bunion?
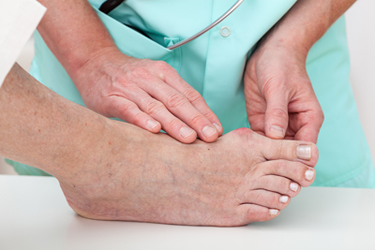
A bunion is considered to be a deformity that can happen for genetic reasons, or from wearing shoes that are too tight. A bunion is a bony growth which forms on the side of the big toe. Severely protruding bunions may cause the other toes to shift toward each other as well, and larger shoes may need to be worn. Some people have corns and calluses that grow on top of the toes, as a result of the friction that is caused when they touch the top of the shoe. Wearing high heels may cause a bunion to form from the limited amount of room the toes have to move in. Relief may be found with mild bunions when a protective pad is worn over them. Some patients have chosen to wear custom-made orthotics, which may help the foot to feel more comfortable in the shoe. If you have a bunion, it is suggested that you consult with a podiatrist who can guide you toward the treatment option that is best for you.
If you are suffering from bunion pain, contact Tanya R. Sellers-Hannibal, DPM of Maryland. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is a Bunion?
Bunions are painful bony bumps that usually develop on the inside of the foot at the joint of the big toe. As the deformity increases over time, it may become painful to walk and wear shoes. Women are more likely to exacerbate existing bunions since they often wear tight, narrow shoes that shift their toes together. Bunion pain can be relieved by wearing wider shoes with enough room for the toes.
Causes
- Genetics – some people inherit feet that are more prone to bunion development
- Inflammatory Conditions - rheumatoid arthritis and polio may cause bunion development
Symptoms
- Redness and inflammation
- Pain and tenderness
- Callus or corns on the bump
- Restricted motion in the big toe
In order to diagnose your bunion, your podiatrist may ask about your medical history, symptoms, and general health. Your doctor might also order an x-ray to take a closer look at your feet. Nonsurgical treatment options include orthotics, padding, icing, changes in footwear, and medication. If nonsurgical treatments don’t alleviate your bunion pain, surgery may be necessary.
If you have any questions, please feel free to contact our office located in Owings Mills, MD . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Bunions
A bunion is a bump that forms at the base of the big toe. Bunions form when the big toe pushes against the next toe, which forces the big toe joint to get bigger and stick out. As a result, the skin over the bunion may start to appear red and it may feel sore.
There are risk factors that can increase your chances of developing bunions. People who wear high heels or ill-fitting shoes are more likely to develop them, in addition to those who have a genetic history of bunions or have rheumatoid arthritis.
The most obvious way to tell if you have a bunion is to look for the big toe pushing up against the toe next to it. Bunions produce a large protrusion at the base of the big toe and may or may not cause pain. Other symptoms are redness, swelling, and restricted movement of the big toe if you have arthritis.
Nonsurgical methods are frequently used to treat bunions that aren’t severe. Some methods of nonsurgical treatment are orthotics, icing and resting the foot, taping the foot, and pain medication. Surgery is usually only required in extreme cases. However, if surgery is needed, some procedures may involve removing the swollen tissue from around the big toe joint, straightening the big toe by removing part of the bone, or joining the bones of your affected joint permanently.
Your podiatrist will diagnose your bunion by doing a thorough examination of your foot. He or she may also conduct an x-ray to determine the cause of the bunion and its severity.
Dealing With Your Child’s Gait Disorder

The gait, which is the way we walk, starts to develop as soon as a child stands up. As they age children go through different stages of gait development, and it is a good idea for parents to monitor these patterns and take note of abnormalities. Three recognizable gait disorders in children are in-toeing, out-toeing, and toe-walking. While in-toeing, also termed pigeon toe, is typical in many children under the age of 3, it also can be caused by a condition where the front of the foot curves inward instead of remaining straight. This can result in a child falling more often than normal. Out-toeing refers to walking with the toes pointed outward instead of straight ahead. It can be the result of flat feet, lower leg misalignment, or hip joint abnormalities. Toe walking is just what it sounds like the child walks on its toes. This can produce tight or shortened calf muscles and may affect balance and cause muscle soreness. If your child displays these or other gait abnormalities, it is suggested that you make an appointment with a podiatrist who can assess the situation and provide guidance on how to handle it.
Making sure that your children maintain good foot health is very important as they grow. If you have any questions, contact Tanya R. Sellers-Hannibal, DPM of Maryland. Our doctor can provide the care you need to keep you pain-free and on your feet.
Keeping Children's Feet Healthy
Having healthy feet during childhood can help prevent medical problems later in life, namely in the back and legs. As children grow, their feet require different types of care. Here are some things to consider...
Although babies do not walk yet, it is still very important to take care of their feet.
Avoid putting tight shoes or socks on his or her feet.
Allow the baby to stretch and kick his or her feet to feel comfortable.
As a toddler, kids are now on the move and begin to develop differently. At this age, toddlers are getting a feel for walking, so don’t be alarmed if your toddler is unsteady or ‘walks funny’.
As your child gets older, it is important to teach them how to take care of their feet.
Show them proper hygiene to prevent infections such as fungus.
Be watchful for any pain or injury.
Have all injuries checked by a doctor as soon as possible.
Comfortable, protective shoes should always be worn, especially at play.
If you have any questions please feel free to contact our office located in Owings Mills, MD . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Bunions
A bunion is an enlargement of the base joint of the toe that connects to the foot, often formed from a bony growth or a patch of swollen tissues. It is caused by the inward shifting of the bones in the big toe, toward the other toes of the foot. This shift can cause a serious amount of pain and discomfort. The area around the big toe can become inflamed, red, and painful.
Bunions are most commonly formed in people who are already genetically predisposed to them or other kinds of bone displacements. Existing bunions can be worsened by wearing improperly fitting shoes. Trying to cram your feet into high heels or running or walking in a way that causes too much stress on the feet can exacerbate bunion development. High heels not only push the big toe inward, but shift one's body weight and center of gravity towards the edge of the feet and toes, expediting bone displacement.
A podiatrist knowledgeable in foot structure and biomechanics will be able to quickly diagnose bunions. Bunions must be distinguished from gout or arthritic conditions, so blood tests may be necessary. The podiatrist may order a radiological exam to provide an image of the bone structure. If the x-ray demonstrates an enlargement of the joint near the base of the toe and a shifting toward the smaller toes, this is indicative of a bunion.
Wearing wider shoes can reduce pressure on the bunion and minimize pain, and high heeled shoes should be eliminated for a period of time. This may be enough to eliminate the pain associated with bunions; however, if pain persists, anti-inflammatory drugs may be prescribed. Severe pain may require an injection of steroids near the bunion. Orthotics for shoes may be prescribed which, by altering the pressure on the foot, can be helpful in reducing pain. These do not correct the problem; but by eliminating the pain, they can provide relief.
For cases that do not respond to these methods of treatment, surgery can be done to reposition the toe. A surgeon may do this by taking out a section of bone or by rearranging the ligaments and tendons in the toe to help keep it properly aligned. It may be necessary even after surgery to wear more comfortable shoes that avoid placing pressure on the toe, as the big toe may move back to its former orientation toward the smaller toes.
Types of Arthritis That Can Affect Your Feet
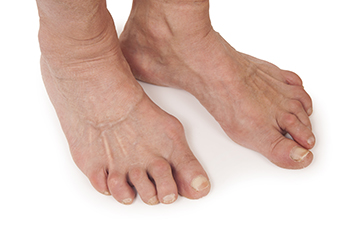
Arthritis is an inflammatory disease that attacks the joints and can cause pain, stiffness, swelling, and bone deformities. There is no known cure for arthritis, but there are many ways of treating the symptoms that allow patients to lead active lives. Because the feet contain 33 joints each, arthritis can negatively impact your daily life, even simply the ability to walk. The main types of arthritis that cause foot problems are osteoarthritis, rheumatoid arthritis, post-traumatic arthritis, and gout. Osteoarthritis is a degenerative disease that erodes the cartilage between the bones of the joint. This causes very painful inflammation and is most common among people 50 and older. It is known as wear and tear disease. Rheumatoid arthritis is a crippling disease where the immune system attacks the body’s cartilage, resulting in deformities. Post-traumatic arthritis can develop after sustaining an injury to the foot or ankle. Gout, which frequently attacks the big toe, is caused by having abnormal amounts of uric acid in the system. To find out more about how arthritis may be causing your foot pain, it is suggested that you consult a podiatrist.
Arthritis can be a difficult condition to live with. If you are seeking treatment, contact Tanya R. Sellers-Hannibal, DPM from Maryland. Our doctor can provide the care you need to keep you pain-free and on your feet.
Arthritic Foot Care
Arthritis is a joint disorder that involves the inflammation of different joints in your body, such as those in your feet. Arthritis is often caused by a degenerative joint disease and causes mild to severe pain in all affected areas. In addition to this, swelling and stiffness in the affected joints can also be a common symptom of arthritis.
In many cases, wearing ill-fitting shoes can worsen the effects and pain of arthritis. Wearing shoes that have a lower heel and extra room can help your feet feel more comfortable. In cases of rheumatoid arthritis, the arch in your foot may become problematic. Buying shoes with proper arch support that contour to your feet can help immensely.
Alleviating Arthritic Pain
- Exercises that stretch the foot can prevent further pain and injury and increase mobility
- Most of the pain can be alleviated with anti-inflammatory drugs, heat, and topical medications
- Massages can help temporarily alleviate pain.
It is best to see your doctor for the treatment that is right for your needs and symptoms. Conditions vary, and a podiatrist can help you determine the right method of care for your feet.
If you have any questions, please feel free to contact our office located in Owings Mills, MD . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.